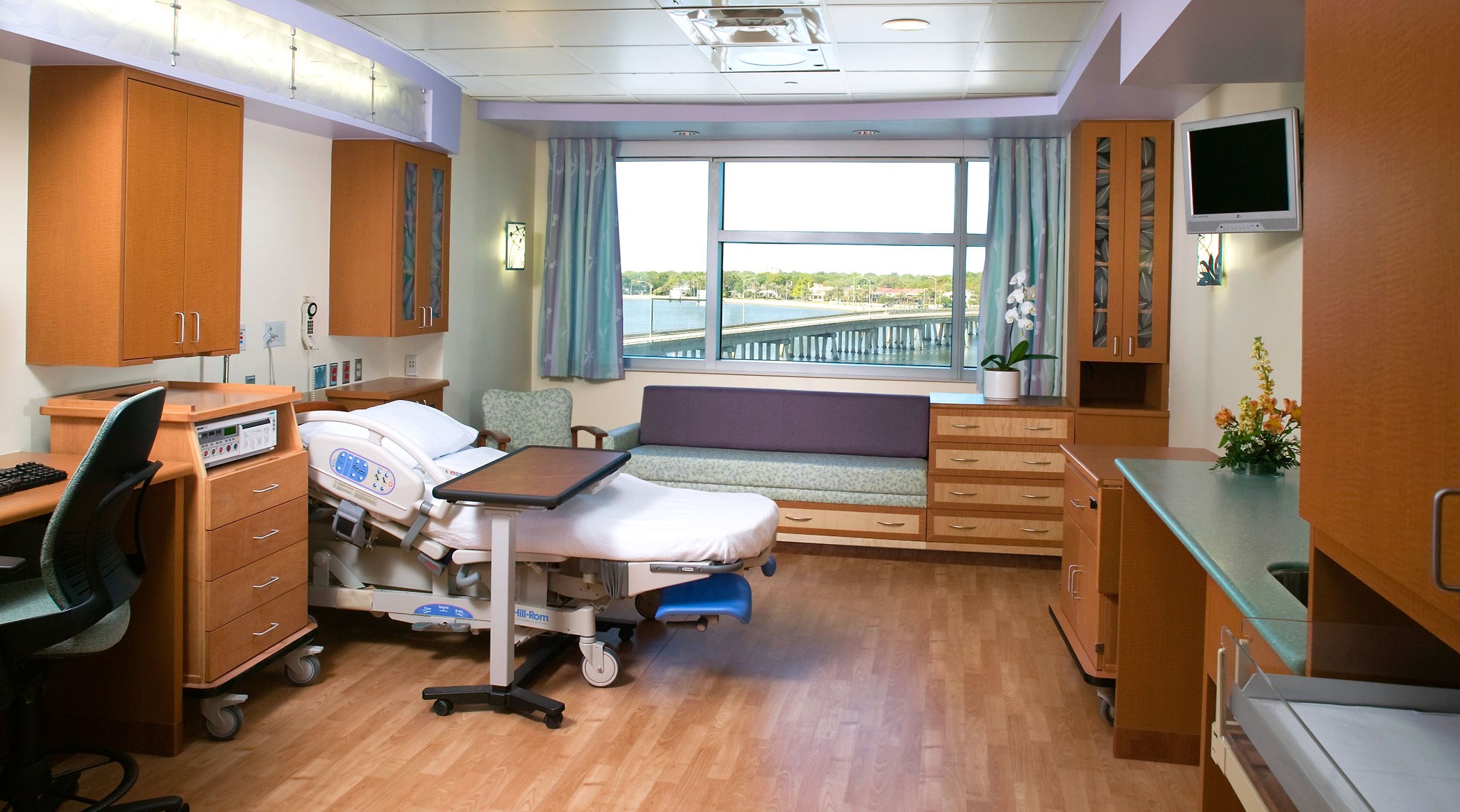
A growing patient population combined with a need to be adequately prepared for a natural disaster meant Tampa General Hospital was running out of room. The healthcare provider called on Gresham Smith to design an expansion on the last unbuilt area on the TGH campus. The resulting 346,000-square-foot, five-story Bayshore Pavilion provides everyday emergency services for the Davis Island Community while being an all-risks-ready care facility in the event of a disaster. The facility serves as a model for future trauma and critical care centers, placing what’s often an afterthought at the forefront of its design.
60
ED exam rooms
346k
square feet
5
stories
Designing Against Disasters
Bayshore Pavilion is located between Davis Island’s access bridge and the seawall, making it especially vulnerable to the effects of hurricanes. Taking guidance from Project ER One, the federally funded initiative to develop all-risks-ready emergency care facilities, our project team incorporated emergency preparedness for medical, natural and man-made disasters. We increased the strength of the structural frames to withstand wind gusts up to 140 miles per hour and with nearly 900 beds, the hospital can eliminate the danger of evacuating large numbers of patients during a storm.An Adaptable Emergency Department
As the only level 1 trauma center in west-central Florida, we made sure our design was flexible and adaptable for surge events. The facility’s entrance uses an airport-style traffic pattern to assist with traffic flow, while the understory can function as an additional arrival point for triage during disasters. We also installed shower enclosures in the event of a mass decontamination. The emergency department has six, 10-room pods, and each room is designed to accommodate two patients during emergencies.Creating a Calming Environment
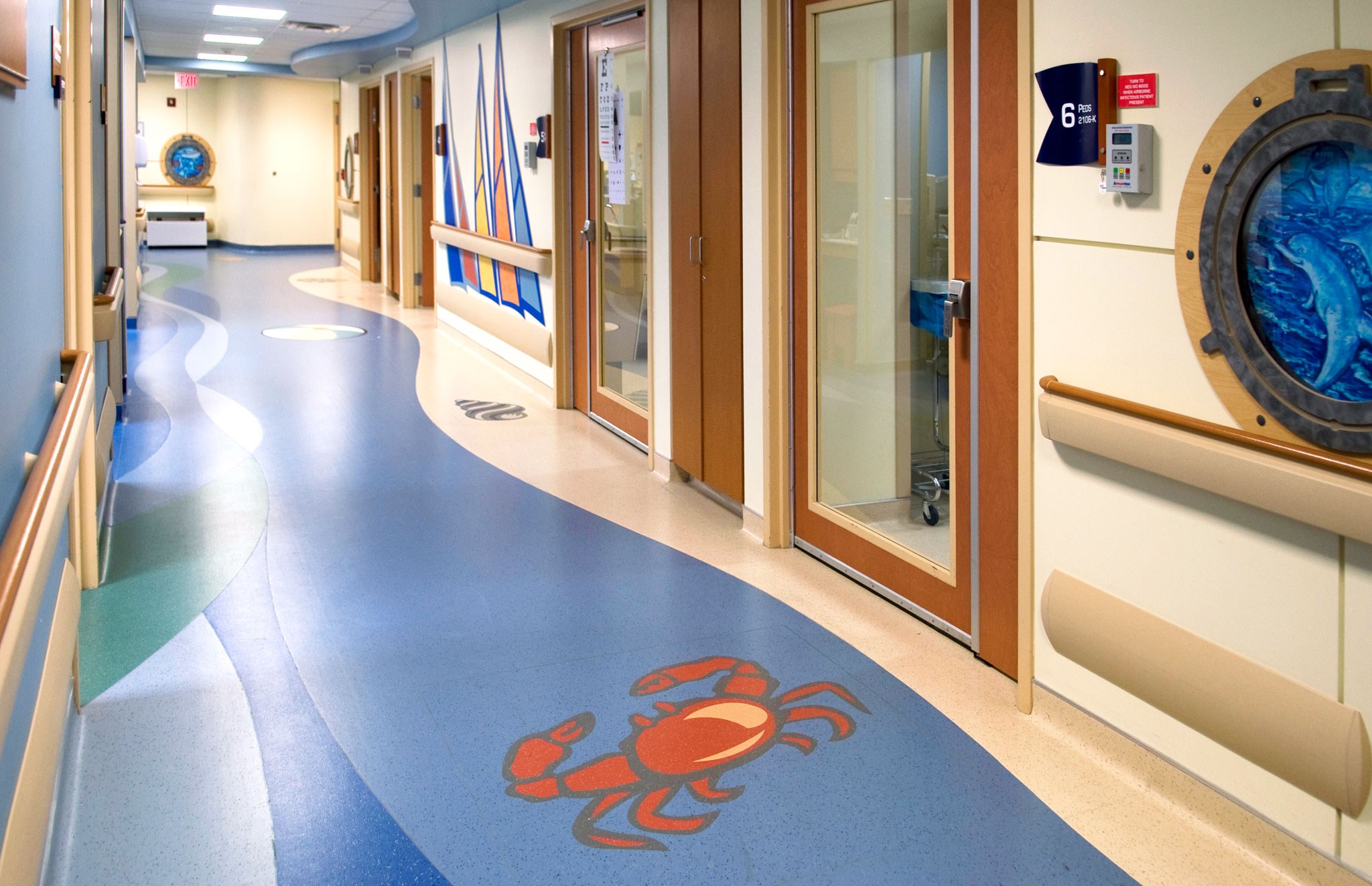
While the building is designed against disasters, our team took special care to create a healing, calming environment. The emergency department’s pediatrics pod is designed with a nautical theme and the nurses’ station resembles a boat with brightly colored flags and waterlines painted on its hull. From undulating soffits on the ceiling to tide-like flooring, we also used soothing colors and oceanic elements throughout the space.Project Contact
Our team designs with genuine care for ingenious solutions.