Each day the news bombards me with stories and images of overwhelmed hospitals and healthcare workers battling COVID-19. While the coronavirus pandemic is full of unknowns and has created more questions than we have answers for, one thing is clear: many of our hospitals lack the flexibility to accommodate the surge of patients and the medical professionals treating them.
As health systems and healthcare providers consider how we can avoid repeating the current national crisis, we have an opportunity to combine healthcare data with design knowledge to analyze how current hospitals are performing and which design elements could play a role in defending against the next health crisis. Keep reading for my thoughts on the hospital spaces and infrastructure we should consider as we think about what’s next.

Administrative Offices and Other High-Density Areas
Just like any workplace, hospitals’ administrative offices and ancillary departments arrange staff in close quarters. However, thanks to the pandemic, dense packing may be a thing of the past. Health systems should examine their workforce mobility before considering whether they need to increase square-feet-per-person in high-density areas, or reduce square footage and offer fewer permanent work spaces and more touchdown spaces for employees who will more frequently work from home. In other departments where working remotely is not an option, such as laboratories and pharmacies, consider spacing and arranging benches, furniture and equipment to reduce cross traffic and provide separation.
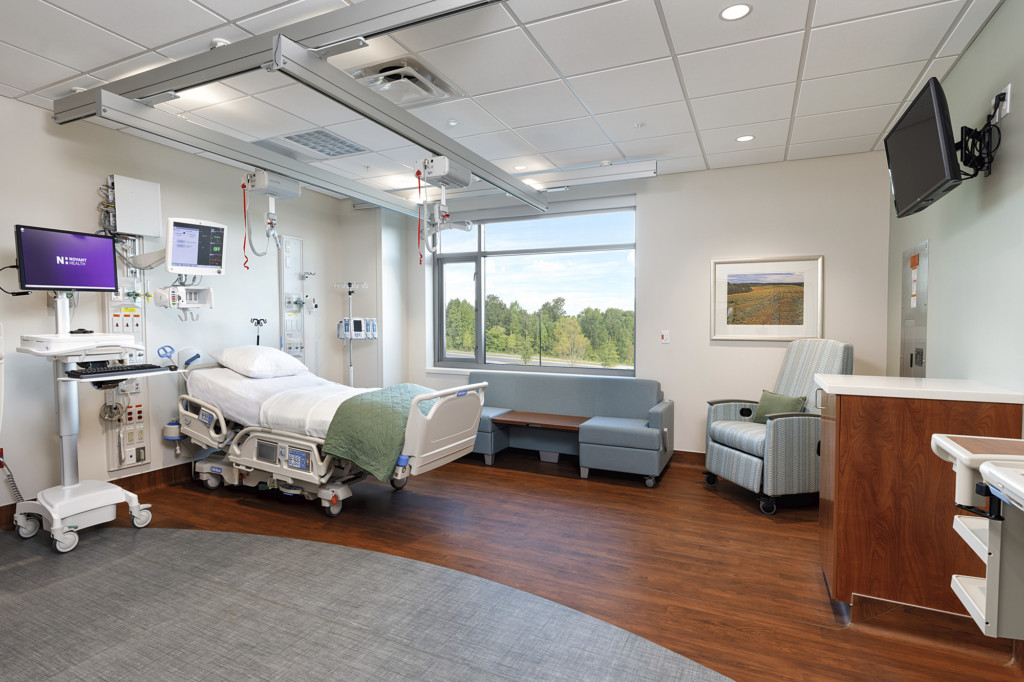
Patient Rooms
While we’ve heard a great deal about intensive care unit capacity, it’s important to remember that not all COVID-19 patients are in the ICU. Many patients have spent their time in typical medical/surgical patient rooms and other non-traditional areas of the hospital, especially now that some doctors are turning to less invasive treatment methods to boost oxygen levels. However, while less invasive, these treatment methods actually pose a greater risk to healthcare workers as leaky masks can expose virus particles.
To mitigate virus spread we should examine the need for additional negative pressure rooms in both ICUs and med/surg units. In addition to designing flexible spaces that can adapt quickly, we should also consider creating units that can be easily segregated into a series of risk zones. Such zones, such as “cold” staff areas and “hot” patient rooms, could reduce the risk to staff by allowing freer movement and reducing the amount of necessary PPE within portions of the unit.

Emergency Department
The pandemic has identified numerous challenges in today’s emergency departments, which act as gateways to our hospitals. The emergency physician is responsible for determining who is at risk, who is infectious and who is not, while at the same time limiting exposure and keeping healthcare staff safe. From the moment patients arrive at the check-in or reception desk, measures should be taken to create separation and contain germs.
While it’s every hospital’s goal to have minimal or zero emergency department wait times, the reality is that there are often significant waits. Future waiting rooms will likely see smaller seating groups surrounded by low walls or decorative panels that provide separation and privacy. Fabrics and seamless finishes that can withstand harsher cleaning solutions will need to be incorporated throughout the space as well.
Additionally, emergency departments’ air change rates should be increased to enable conversion to negative pressure relative to adjacent hospital zones, as well as allow the emergency department to be 100% exhausted with no air recirculation. Increasing air change rates and exhaust would help the ED mimic the pressures in isolation rooms and should especially be considered for all waiting areas where potentially infectious patients could be present.

Pharmacy
One of the largest threats to patient care is a drug shortage. In addition to creating a system-wide drug shortage plan, health systems should decide if high-demand medications and other needed supplies will be stockpiled onsite. Additionally, to enhance communication with physicians regarding drug availability and applications, design professionals should consider adding pharmacist touchdown stations on bed floors so that they can work hand-in-hand with providers during surge events.
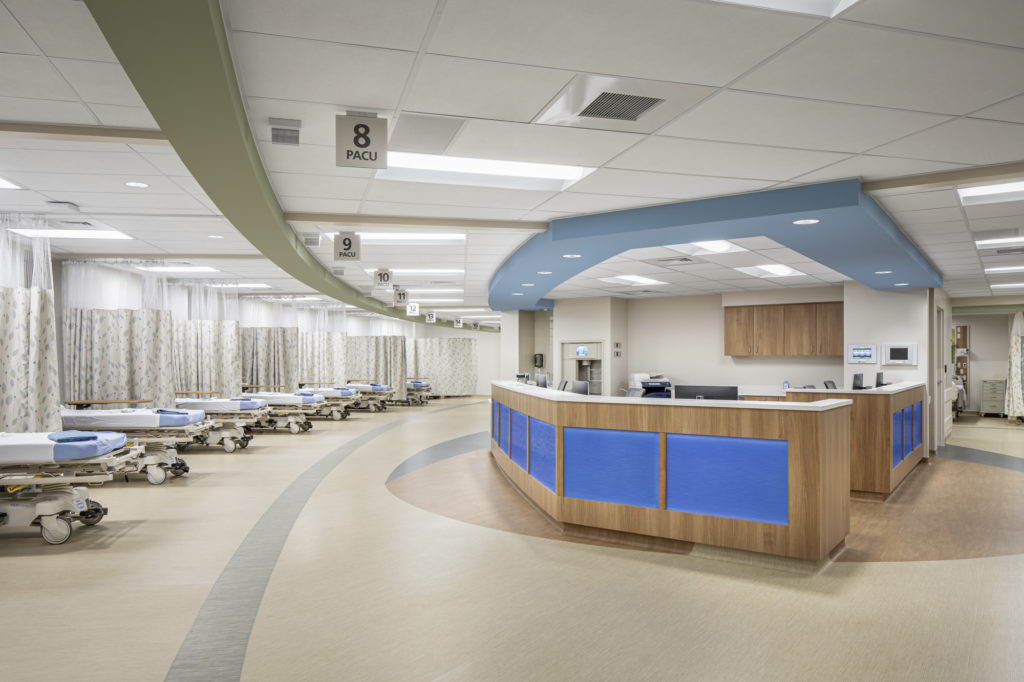
HVAC
Heating, ventilation and air conditioning systems throughout hospitals are space/unit specific, making it difficult and expensive to change or enhance its use for the space it serves. In many facilities, the lack of oxygen outlets has prohibited the use of available space as patient care areas. As designers, we should consider integrating more robust HVAC infrastructure so that spaces can be converted as quickly and efficiently as possible, enabling providers to create temporary patient treatment areas safe for patients and staff.
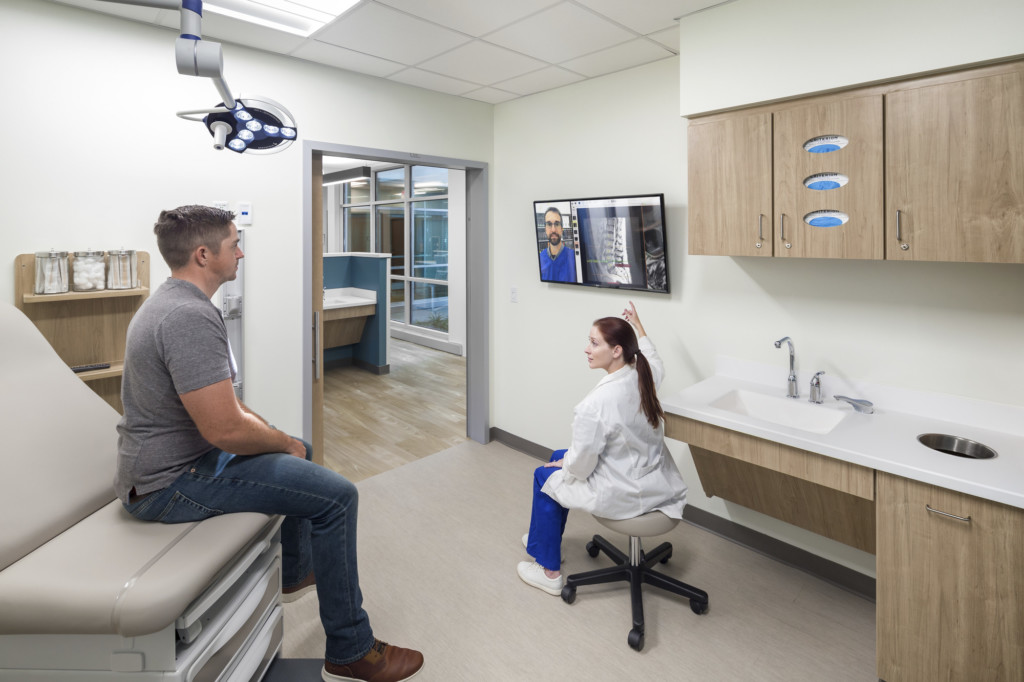
Telehealth
Health systems are pushing patients towards virtual visits for both virus containment and cost reduction. As providers begin implementing more telehealth services post-pandemic, hospitals should consider how the increased activity will affect their IT infrastructure. Additionally, it may be wise to create designated rooms for providers to use during telehealth visits.
As health systems take it one day at a time, our job as design professionals is to remember that the coronavirus pandemic will have long-term implications on how we design hospitals. From being proactive with patient unit design and strategically locating supplies and PPE to considering technology’s impact, we have a responsibility as designers to use this experience to inform the future of healthcare design and defend against devastating health events.