
“Hospitals of the future” has been the hot topic of conversation around the proverbial office watercooler. My two cent contribution to these conversations usually comes in the form of my assertion that the pragmatics of healthcare architecture can sometimes hold us back from truly imaging what the future of healthcare architecture could be. Take for example the scientists who spend a great deal of their time exploring “predictions and possibilities about the future.” These scientists, otherwise known as “futurists,” have singled out Artificial Intelligence (AI) as a source of considerable benefits to the way that healthcare services are delivered. But why the focus on AI and why now? Accenture Analytics sites the ability of AI to deliver cost savings in an era marked by “rising labor costs, digital expectation from consumers and increasing demands of interoperability.” This post explores three areas where AI has the potential to impact healthcare delivery services as well as the role that Value-Added Design plays in improving diagnostics, reimagining patient-caregiver interaction and improving the business of healthcare.
Improving Diagnostics
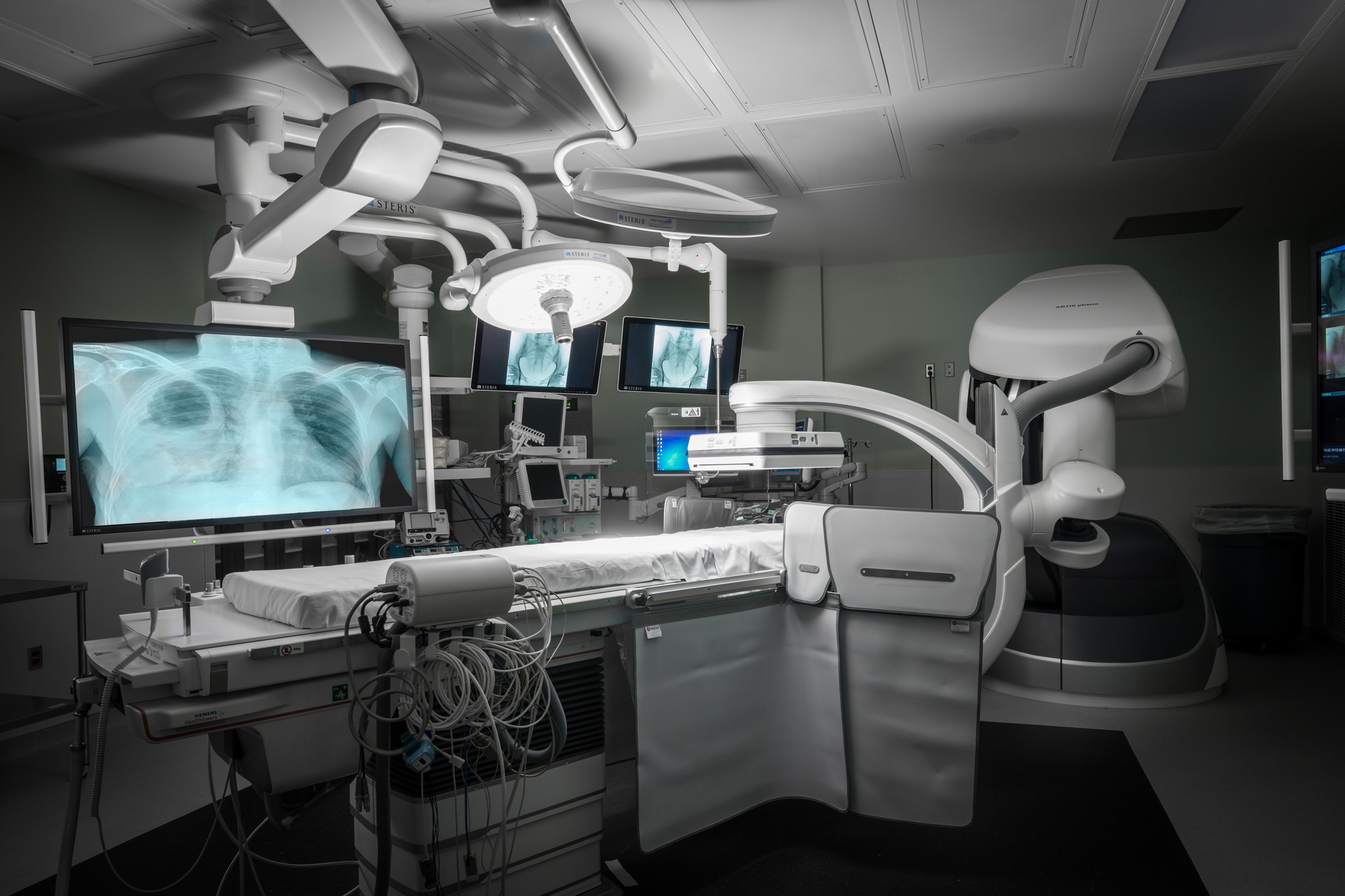
Virtual pattern recognition as well as the ability to analyze and learn (“deep learning”) from historical cases and thousands of data-base images, are just two aspects of AI that can significantly impact diagnostic accuracy. Given hospital reimbursements are tied to quality, the financial benefit to providers are obvious. But it’s the moral and emotional aspect of patient care that perhaps most benefits from introducing AI into the patient care mix. Patient Safety and Integration of Technology are cornerstones of our Value-Added Design services. Integrating AI technology in the spaces we design can help support patient safety. Providers benefit from the timely, exhaustive analysis that AI can provide. It will provide a broader set of client experiences and treatment options to allow providers to better customize course of treatments and thereby position providers as both state-of-the-art and human-centric.
Reimagining Patient/Caregiver Interaction
Regardless of improved accuracy gains, caregivers may struggle with the idea of a computer logic qualifying decisions that have for decades relied heavily on instinct and medical intuition. What exactly does this mean for healthcare delivery? The possibilities are numerous, from harnessing the power of AI to develop specialized treatment plans for patients to precision medicine focusing on genetics to reducing the time needed to develop new treatment drugs. One of the most interesting possibilities lies in how AI can affect the interaction between patients and caregivers. Imagine being treated by a “virtual nurse” that can take your entire personal medical history, document your symptoms, compare them to thousands of similar cases and have a diagnosis ready for the doctor to confirm at the time he walks into the room. Can wait times be reduced by this scenario? Can patient satisfaction and efficiency increase? Can the accuracy of diagnosis be improved under this scenario? All indications point towards yes. The Human Experience, and the idea that AI does not replace, but augments caregiver capabilities, is the thread that helps tie AI and patient/caregiver interactions. Similarly, GS&P’s Value-Added Design focus on the Human Experience serves to augment the patient/caregiver communication by way of healing environments that lead to positive patient experiences to help generate improved patient outcomes.

The Business Side of Things
I recently sat in a presentation focused on AI and its impact on our economy. The speaker began the presentation by assuring the audience that the robots typically associated with AI were in fact “not out to kill us all.” In fact, the opposite is true. AI, harnesses the power of technology to support and improve the work that humans already do by reducing repetitive tasks, automating routines and improving decision making through a focus on data and evidence. This has tremendous potential to impact on the bottom line. Consider that robotic surgery, for example, offers reductions on average length of stays. Also consider improvements to the bottom line that can be gained by streamlining administrative workflows that offer time saving to patients, nurses and doctors alike. And as we all know, time is money. Designers are also starting to use AI to optimize design. We can work to address providers’ bottom-line concern by actively working to improve our clients’ Operational Efficiencies. GS&P’s Value-Added Design initiative promotes the active use of tools that document operational models thereby uncovering areas where efficiency gains can be achieved. We support our clients’ Operational Efficiency efforts through the use of technology and computer simulations that allow us to right-size their facilities, including AI-supported computational design. We enhance these efforts by employing process improvement principles, such as Lean Six-Sigma, to explore how clients can reduce operational waste while also building operational efficiency thus contributing to an improvement to their bottom line.

Bringing It All Together
The “hospital of the future,” will continue to be affected by the same changing payment landscapes and regulatory considerations that affect today’s hospitals. The combination of these and other factors will continue to place financial pressure on operational assets, the bottom line and our clients’ ability to explore opportunities for growth. Science and technology can play a crucial role in alleviating some of these pressures. Artificial Intelligence, and its introduction into the patient/caregiver mix, is already showing signs of promise in the areas of diagnostics, patient/caregiver interaction and business. Real dividends for clients can be gained, and additional operational improvements achieved, in those cases where science, technology and smart design converge.
