As a designer of hospitals, I have always been curious about how nurses in the med/surg nursing unit spend their shifts, and how the design of these units impacts the delivery of patient care. In 2016, I had the opportunity to shadow a med/surg nurse during most of her daytime shift and recounted what I learned from that direct observation in my blog post 8 Design Lessons from Shadowing a Nurse.
As chronicled in the blog, although I had a solid grasp of the fundamentals of the of the typical nursing routine in these types of units, during those eight hours of observation, I learned some things that only a real-time experience could provide. I walked away from that shadowing session resolute that design professionals need to see for themselves what clinical staff actually do on the front lines.
As I was not able to get to the unit until late morning during that first observation, I returned a few months later on a weekend to observe the morning shift change. This time, I shadowed a nurse I’ll call “Cammie,” who was incredibly gracious in allowing me to follow her around with stopwatch and notebook in hand. In today’s post, I share some of those observations and design lessons learned.
It’s All About Timing
As a non-clinical person, I assumed that weekends would be prime time for families to visit the med/surg nursing unit. However, the activity level in this particular unit was much lower on the weekend than on a weekday.
One of my first lessons learned from Cammie is that the rhythm of the unit is specific to the community it serves. When family members are forced to decide between missing work and supporting their loved one, they will prioritize visit times to when the doctors are present and procedures are scheduled. Although there is less demand on the weekend for nurses to prepare patients for procedures, the absence of family members and the supplemental care they often provide means there is no one else to assist with routine patient care.

Special Challenges of Isolation Care
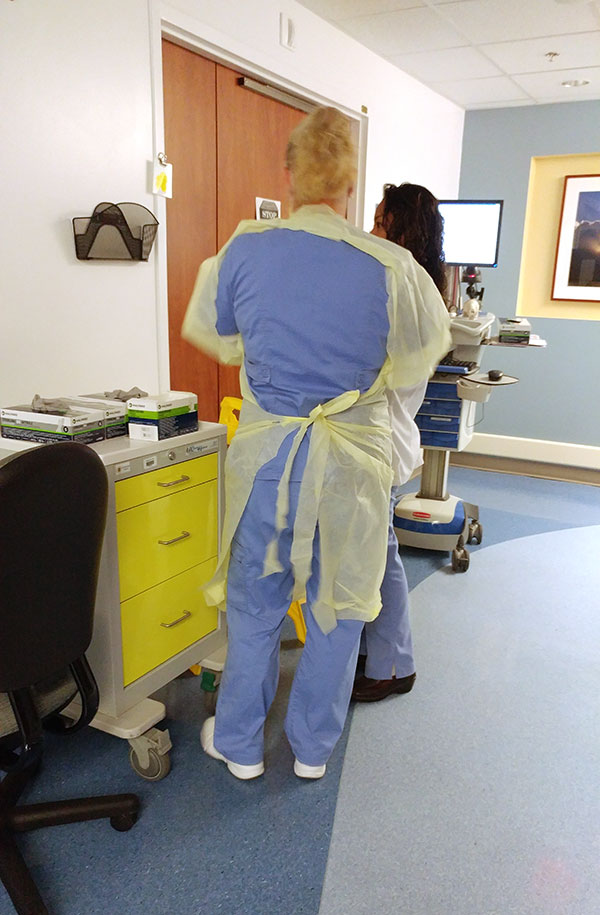
One of Cammie’s patients who was placed under isolation was also obese and required a transfer lift. I watched Cammie put on and remove her gown repeatedly and realized that it’s one thing to understand this concept, but quite another to actually observe it. Over a four-hour period, Cammie gowned up a total of five times. The dietary staff gowned up twice; once to deliver breakfast, and then again to pick up the tray. The respiratory therapist also had to gown up for protection.
Because of the patient’s weight, Cammie required assistance from the charge nurse, which meant more gowning. Ten gowns were used during a four-hour period and this was on a weekend, which was slower. During the week, the number of gowns used is most likely higher because of rounding physicians and visiting family members. As the isolation gowns and masks are both hot and uncomfortable, the time needed to dress and undress really adds up on a busy day. The personal protective equipment (PPE) for the isolation room was kept in a large cart parked in the corridor outside the patient room. It made me realize it would not have been feasible for Cammie to walk to the far end of the unit to fix flyaway hair, for example, or to check her appearance after taking off the gown. This got me thinking, perhaps designers should provide a small mirror when we design built-in PPE cabinets.
Location, Location, Location
“Angela,” the first nurse I shadowed, was assigned to patients at the busy entry corridor of the med/surg nursing unit. All the unit’s traffic passed by these rooms, including visitors, social workers, dietary aides, hospital service workers and residents making their rounds. In contrast, Cammie’s patients were in rooms along one of the back corridors. Unless someone needed to enter one of these rooms or to speak with her, they did not venture into this part of the unit.
Fortunately, Cammie was assigned to patients in adjacent rooms and spent most of her day close by. However, studies suggest that patients in rooms farther from the main nurse station have higher mortality rates, even though they tend to prefer those rooms because they are quieter. This has to be taken into consideration when designing med/surg nursing units. To increase patient comfort, back-of-house traffic should be separated from patient areas as much as possible. Patient rooms located near a central nurse station require additional acoustic measures.
The contrast between the bustling entry corridor and the more isolated back corridor on this small unit was dramatic. On new projects, we can use simulation modeling to track travel distances, milestone times, wait times and throughput. Utilizing a digital prototype for proposed floor plans also helps us conduct better opportunity cost analyses and identify gaps, bottlenecks and efficiencies. By testing traffic flow in the model, we can create evenly distributed traffic patterns that eliminate extreme differences between patient rooms. Ideally, every patient room would be quiet and have equal proximity to staff.

Work Styles and Workplace Strategy
In healthcare design, the layout of space is based on procedures and best practices, which makes it tempting to think of healthcare delivery as a regimented process. In reality, each person working within the unit has a different work style, and the environment should be designed to support personalization while at the same time reinforcing and enhancing the organization’s goals.
How Angela spent her time
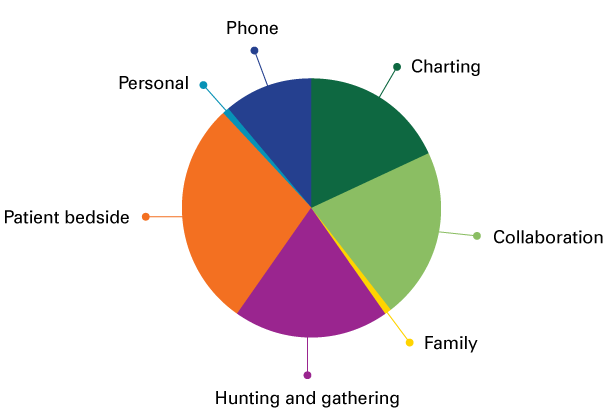
How Cammie spent her time
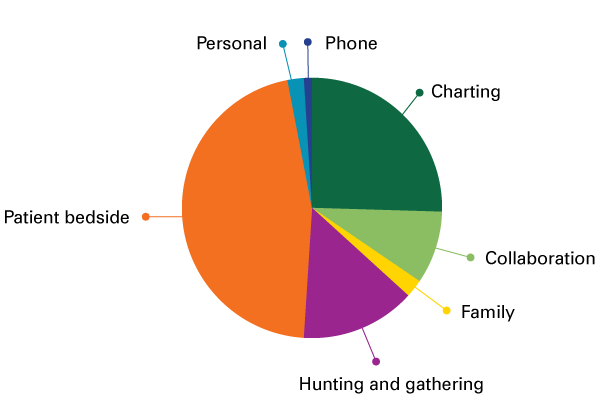
To that point, the two nurses I shadowed had very different temperaments and methods. Although both clearly cared for their patients, Angela was more social with other staff members, while Cammie had a more focused, heads-down approach. Additionally, Angela visited her patients more frequently, but Cammie stayed with them for longer periods.
It was interesting to observe that the younger nurses asked Angela for advice throughout the afternoon, while Cammie seemed happy to work autonomously, exchanging a few words every now and then with the charge nurse. An exceptional med/surg nursing unit design would allow nurses like Angela to teach others and feel connected to her team. Nurses like Cammie would be able to focus with quiet concentration without being isolated.
Ultimately, we may work with the leadership of an organization to develop the vision for a project, but talking with and observing a broad range of people within the organization is critical. This “frontlines” perspective allows designers to apply the vision in a way that empowers staff to carry it out.